Published: 2 June 2016
Publications
The Ionic Truth about Hyponatraemia
Prescriber Update 37(2): 19-21
June 2016
Background
Hyponatraemia is the most common electrolyte disturbance seen in clinical practice1. It is defined as a serum sodium concentration of less than 135 mmol/L1.
Hyponatraemia is primarily a disorder of water balance usually associated with a disturbance in the hormone that regulates water balance, vasopressin (also commonly called antidiuretic hormone [ADH])1.
Symptoms of Hyponatraemia
Symptoms can range from mild and non-specific to severe and life-threatening (Table 1). The severity of symptoms depends on many factors including the duration of the condition, serum sodium levels and the acute or chronic nature of onset2.
Severe symptoms are caused by cerebral oedema and increased intracranial pressure due to the movement of water into brain cells1.
Table 1: Symptoms of hyponatraemia by severity1
| Severity | Symptoms |
|---|---|
| Moderate | Nausea without vomiting Confusion Headache |
| Severe | Vomiting Cardiorespiratory distress Abnormal and deep somnolence Seizures Coma (Glasgow Coma Scale ≤8) |
Determining the Cause of Hyponatraemia
Hyponatraemia occurs when the patient has excess free water relative to serum sodium levels2. It can be categorised according to the patient's extracellular fluid volume status1,2.
- Euvolaemic (normal fluid status): Possible causes include medicines, syndrome of inappropriate ADH secretion (SIADH), central nervous system disorders, secondary adrenal insufficiency, pulmonary diseases, hypothyroidism and primary polydipsia.
- Hypervolaemic (fluid overload): Possible causes include heart failure, nephrotic syndrome, renal failure, Cushing syndrome and saline infusions.
- Hypovolaemic (fluid depletion): Possible causes include vomiting, diarrhoea, cerebral salt wasting, pancreatitis, burns, primary adrenal insufficiency and the use of diuretics.
Additional laboratory tests may be useful. These include urine osmolality, serum osmolality and urine sodium concentrations2. The cause of hyponatraemia in many patients may be unclear, but it recurs in the context of intercurrent illness.
Hyponatraemia in Older People
Patients presenting with hyponatraemia tend to be over 80 years of age, female and living in long-term care facilities3.
Sodium imbalances are particularly common in older people partly because of the normal aging process that affects the body's ability to maintain water and sodium homeostasis3.
Causes of hyponatraemia in older people include:2
- structural changes in the kidney leading to functional declines including decreases in glomerular filtration rate, creatinine clearance and renal plasma flow
- hormonal changes related to aging
- medicines (see Medicine-induced Hyponatraemia)
- low dietary sodium intake.
Medicine-induced Hyponatraemia
There are many medicines that can cause hyponatraemia through several pathological mechanisms (Table 2).
Diuretics are one of the most common causes of hyponatraemia4. Diuretic-induced hyponatraemia is mostly caused by thiazides; loop diuretics are rarely associated with hyponatraemia4. Selective serotonin reuptake inhibitors (SSRIs), antipsychotics and non-steroidal anti-inflammatory drugs (NSAIDs) are also known to cause hyponatraemia4.
There have also been reports of hyponatraemia following treatment with ACE inhibitors, antibiotics (eg, co-trimoxazole and ciprofloxacin) and proton pump inhibitors4.
Medicine-induced hyponatraemia usually develops within the first few weeks of starting treatment4. A combination of medicines may be responsible for hyponatraemia rather than just one medicine. The sodium lowering potential of medicines added to a patient's treatment regimen that already contains such a medicine should be considered.
Table 2: Medicines known to cause hyponatraemia and their underlying mechanisms4
| Mechanism | Examples |
|---|---|
| Medicines affecting sodium and water homeostasis | |
Diuretics:
|
|
| Medicines affecting water homeostasis | |
| Increased hypothalamic production of ADH | Antidepressants:
|
Antipsychotics:
|
|
Antiepileptics:
|
|
Anticancer agents:
|
|
Miscellaneous:
|
|
| Opiates | |
| Potentiation of ADH effect | Antiepileptics:
|
Anticancer agents:
|
|
| Non-steroidal anti-inflammatory drugs (NSAIDs) | |
| Reset osmostat | Antidepressants:
|
Antiepileptics:
|
|
New Zealand Cases
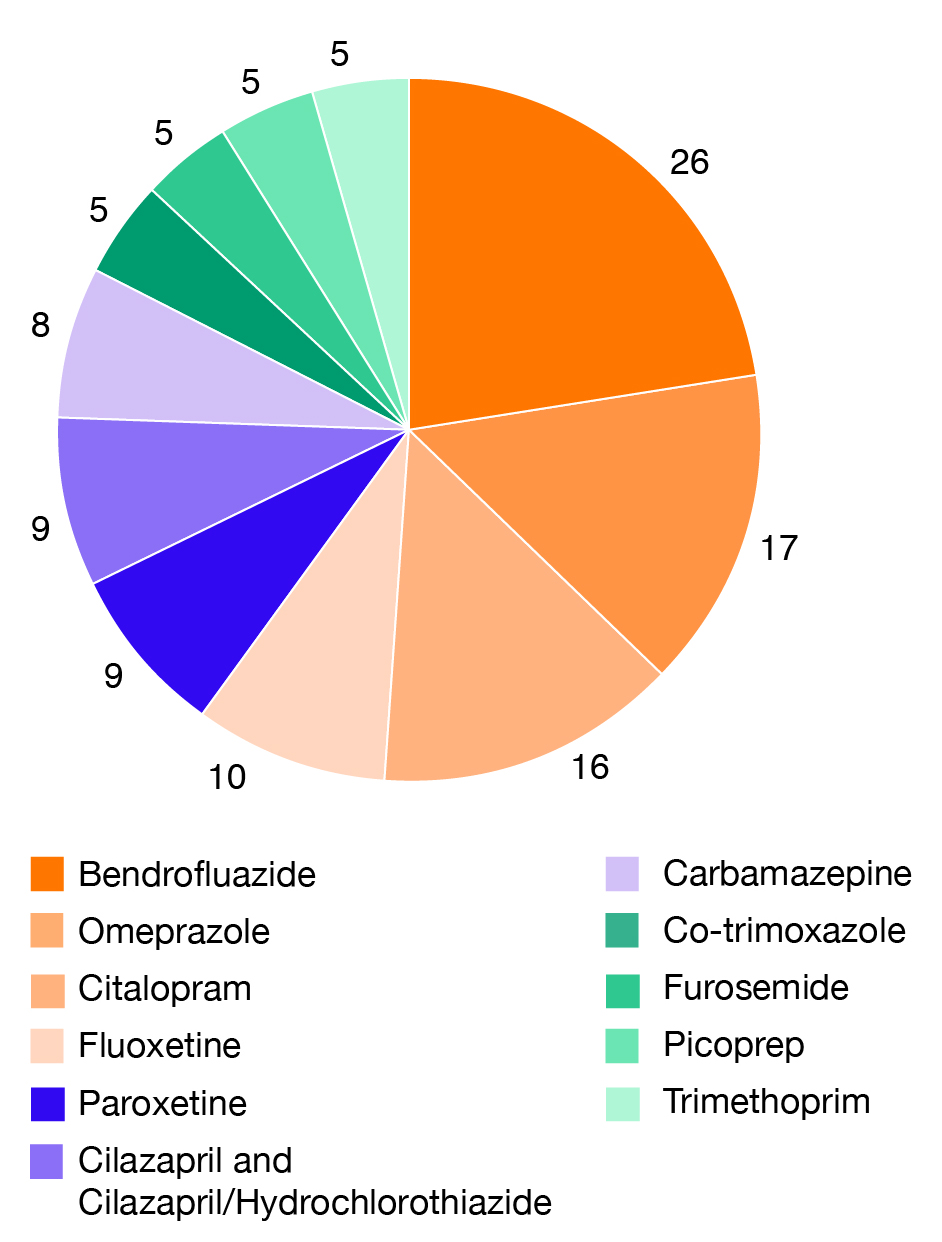
The Centre for Adverse Reactions Monitoring (CARM) received 146 reports of hyponatraemia from 2006 to 2015. Of these, 93 cases involved one suspect medicine and 53 involved multiple suspect medicines. The most frequently reported medicines are summarised in Figure 1.
In these cases, hyponatraemia was more common in females (74.7%) compared to males (25.3%) and the average age was 72 years.
Management
Prompt intervention is important to prevent fatalities2. Treatment may include oral fluid restriction, intravenous administration of hypertonic saline and treating underlying conditions while taking the patient’s volume status into account2.
If medicine-induced hyponatraemia is suspected, the medicine(s) should be withdrawn. Hyponatraemia usually resolves within two weeks of stopping the offending medicine(s)4.
Please continue to report any adverse reactions to CARM. Reports can be submitted on paper or electronically (https://nzphvc.otago.ac.nz/).
References
- Spasovski G, Vanholder R, Allolio B, et al. 2014. Clinical practice guideline on diagnosis and treatment of hyponatraemia. European Journal of Endocrinology 170(3): G1-G47.
- Moran D, Fronk C, Mandel E. 2014. Managing hyponatremia in adults. Journal of the American Academy of Physician Assistants 27(4): 23-29.
- Schlanger LE, Bailey JL, Sands JM. 2010. Electrolytes in the aging. Advances in Chronic Kidney Disease 17(4): 308-319.
- Liamis G, Milionis H, Elisaf M. 2008. A review of drug-induced hyponatremia. American Journal of Kidney Diseases 52(1): 144-153.





